Caring for Under-resourced Populations and Improving Health Access - The PA Perspective
- Jennifer Vonderau
- 2 hours ago
- 3 min read
By Jen Vonderau | 4/23/2026
The Physician Associate/ Assistant (PA) profession was founded on a mission of extending healthcare access, born from an expansion of military service to ensure that healthcare reached every community. Today, that mission is more critical than ever.
The World Health Organization (WHO) predicts a shortage of 11 million health care providers by 2030, and in the United States, the Bureau of Labor Statistics anticipates a deficit of over 70,000 primary care providers by 2038 (WHO, BLS). As our healthcare system faces increasing strain, the PA workforce - growing annually to over 200,000 practicing PAs - is one solution to provider shortages and the growing health needs of under-resourced populations (NCCPA).
Whether in rural clinics or urban community health centers, PAs are no longer just physician extenders: PAs are the connective tissue between vulnerable patients and the care they deserve.
A Clinical Force for Community Health
PAs are essential clinical providers who expand access across all environments. The Health Resources and Services Administration (HRSA) defines areas of the US that are underserved and/ or under-resourced by population or geographic area.
HRSA codes these designations as Medically Underserved Areas/ Populations (MUA/P) and Health Professional Shortage Areas (HPSAs). An MUA/P is defined as an area with insufficient primary care providers, high infant mortality, poverty, or an older adult population. An HPSA is an area with insufficient providers of primary medical care, dental care, or mental health care; an HPSA may be designated according to geography, population, or facilities (NCCPA).
A Federally-qualified Health Center, or FQHC, serves a designated underserved area or population. In Community Health Organizations and FQHCs, PAs bridge the gap for underrepresented populations. These roles are often highly impactful, as PAs address mental health issues and chronic diseases for individuals who might otherwise avoid care due to financial or social barriers.
The PA impact in extended care to these populations measurable (NCCPA):
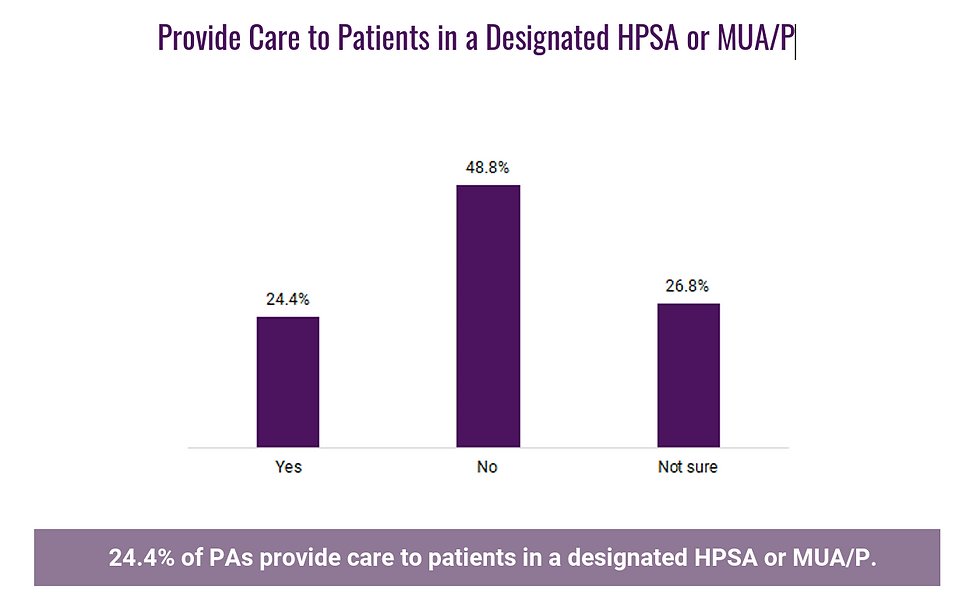
24% of PAs practice in a designated MUA/P and/ or HPSA
A single PA sees 100 patients a week as a primary provider, on average
The profession conducts roughly half a billion patient evaluations annually
PAs see approximately 11 million patients every week
Removing Financial Barriers to Service
For many new graduates, the desire to work in public service is often at odds with the reality of high student loan debt. Urban under-resourced roles may pay less than private practice, but there are robust programs designed to help PAs follow their passion for community health without financial penalty:
Program Type | Description |
Offers substantial loan repayment in exchange for a two-year commitment to serve in an HPSA. | |
Forgives remaining loan balances for full-time employees of qualifying non-profits after 120 payments. | |
State-Specific Grants | Many states offer unique loan repayment incentives for clinicians working in their most underserved regions. |
HRSA Grants | Programs like the "Be the CHANGE" grants provide funding for PAs to lead community-based health initiatives. |

Advocacy: Increasing PA Presence
Improving access isn't just about showing up to the clinic; it's about changing the laws that govern how we practice. Legislative victories like Optimal Team Practice (OTP) are essential for removing administrative burdens that can limit a PA’s ability to serve a community autonomously.
By advocating for collaborative rather than strictly supervised practice, PAs can more effectively fill gaps in healthcare deserts where physician oversight may be difficult to secure. This structural shift allows us to move from being extensions of care to equitable and strategic leaders of the modern healthcare team.
The Road Ahead
The physician workforce is growing, but it is growing slowly (BLS). The US and its diverse and geographically dynamic populations require PAs and advanced practice providers (APPs) to reach all communities.
To read more about the PA role in an FQHC, sign up for our free monthly newsletter PA Jobs Continuing Mentorship & Education! The April edition features James Pecard, MMS, PA-C, a PA with years of practice experience in an FQHC.
Interested in finding a role in community health?
Check out our PA Jobs by Specialty page
See our PA Jobs by Specific Populations page
Explore our resources on Scholarships and Loan Forgiveness
%20PNG.png)



Comments